#treatment
Vivostat PRF Biological Glue
Vivostat PRF (Platelet Rich Fibrin) is an autologous, bioabsorbable, bioactive, biological glue that is now available for various uses in modern knee surgery:
- Autologous – means that the glue comes from the patient’s own blood, and not from donors.
- Bioabsorbable – means that the glue just dissolves gradually with time (just like a normal blood clot).
- Bioactive – means that the PRF doesn’t act just purely as a mechanical glue: it also actively promotes tissue healing through release of growth factors from the high concentration of platelets that it contains.
- Biological – means that the glue is not synthetic, but it is ‘natural’ (it comes from the patient themselves).
I have been using Vivostat PRF since 2014 now in the knee surgery that I undertake, as an important part of a number of specific procedures:
- Articular cartilage grafting: the Vivostat PRF acts as a mechanical glue to hold Chondrotissue articular cartilage grafts in place. At the same time, it also seals over the surface of the graft to prevent loss of cells from the graft (from cells simply being ‘washed away’ by the joint fluid). It also promotes early healing of the cartilage graft through release of growth factors.
- Meniscal allograft transplantation: here, the Vivostat PRF is used as a sealant around the periphery of the graft, to help promote rapid healing of the meniscal allograft to the patient’s capsule.
- Meniscal repair: in some more difficult meniscal repairs, Vivostat PRF can be used to augment the repair, to increase the probability of success healing.
- ACL reconstruction: here, I spray Vivostat PRF up/down the femoral/tibial bone tunnels in order to seal the tunnels (to prevent synovial fluid getting into the tunnels, which can inhibit healing) plus I also spray Vivostat PRF over the ACL graft itself, to try and encourage rapid revascularisation and healing of the ligament.
- Knee replacement surgery: Vivostat PRF can also be used as a fibrin sealant for knee replacements, to reduce bleeding from exposed cut bone surfaces and cut tissue edges, which reduces post-operative swelling and pain, which then improves post-op recovery and rehabilitation.
How is Vivostat PRF obtained?
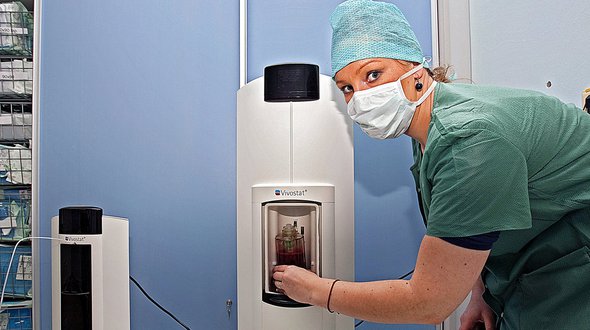
Vivostat PRF is obtained by taking a small amount of blood (120ml) from the patient’s arm once they are asleep in the anaesthetic room. The blood is then spun in a special machine (the Vivostat ‘Tower’) in theatres, which produces approximately 5ml of PRF, which is ready for use within 1/2 hour in theatres (which means that it is available by the time that it is actually needed, which is normally towards the end of any surgical case).
Use of Vivostat PRF in other surgical specialties
The first time Vivostat PRF was used in a knee in the UK was within my practice in London back in 2014. However, prior to this, Vivostat PRF was already being used in a number of other surgical settings in different specialities, including:
- Vascular/Cardiac Surgery: for sealing vascular anastamoses
- Plastic Surgery: for getting chronic wounds to heal
- Neurosurgery: for sealing dural closure and preventing CSF leakage
- Hepatic Surgery: to seal over the raw surfaces of liver tissue to prevent bleeding and bile leakage in major liver resections
- Fasciomaxillary surgery: for the treatment of temporomandibular disease.
How is Vivostat PRF applied?
One of the many advantages of Vivostat PRF is the applicator system, which is very versatile, and which allows the PRF to be sprayed onto tissues in a very controlled fashion.
For open cases, a ‘pen’ applicator is supplied, which allows a jet / spray of PRF to be applied evenly to tissue surfaces.
For arthroscopic (keyhole) cases, the Vivostat applicator tube can be passed up a Frazier sucker, allowing accurate application directly onto required areas under direct arthroscopic control.
Articular cartilage grafting
Vivostat PRF is used in articular cartilage grafting in the knees as:
- a mechanical glue, to hold the graft in place,
- a sealant, to cover over the surface of the graft and to keep cells in place within the cartilage graft, preventing cells simply being washed away by the arthroscopy irrigation fluid or, later, by the patient’s own synovial joint fluid, and
- to promote early healing of the graft, due to the growth factors that are released from the high concentration of platelets.
Meniscal repair
Whether or not a meniscal tear is repairable depends on a number of various factors, not least being whether there is a good blood supply to the part of the meniscus that is torn. Blood vessels supply only the outer 1/3 of the meniscus, with the inner 2/3 being ‘avascular’. Without a decent blood supply tissue cannot heal.
In some complex meniscal tears and/or in meniscal tears in younger patients (especially young athletes) where preservation of the meniscus is critical, a meniscal tear can be augmented by spraying the repair over with Vivostat PRF.
The meniscus is ‘trephined’, which involves poking multiple holes through the meniscus with a needle, which creates little vascular access channels for the peripheral capillaries to bleed into the tissue, which then promotes healing. Vivostat PRF can create a barrier / sealant, that keeps the blood within the meniscus and that prevents the synovial fluid from washing it away. The growth factors released from the platelets in the PRF can also promote healing.
Meniscal transplantation
Meniscal transplantation involves the surgical implantation of a new meniscus from a donor into the knee of a patient who has previously had their meniscus removed due to them having had an irreparable meniscal tear. Replacing a missing meniscus can reduce pain, improve function, slow down the progression of wear and tear, and help a patient keep their knee going for longer, delaying bigger operations such as artificial joint replacement surgery.
Vivostat PRF is an excellent adjunct to the surgical technique of meniscal transplantation. The PRF can be sprayed around the periphery of the new meniscus, underneath it and over the insertional ligament attachment sites to promote more rapid healing of the graft.
Biological augmentation of ACL grafts
In my practice, I routinely use Vivostat PRF with my ACL reconstructions. I spray the PRF up the distal end of the femoral tunnel, over the front and around the back of the intra-articular portion of the graft, and also copiously around the distal end of the tibial tunnel too. This is a cheap, safe, autologous method of reducing post-op bleeding, swelling and pain, and improving the biological healing of grafts.
A recent publication in the The Orthopaedic Journal of Sports Medicine has reported the results of the first formal study looking at the use of Vivostat PRF in ACL surgery:
Does the application of platelet-rich fibrin in anterior cruciate ligament reconstruction enhance graft healing and maturation? A comparative MRI study of 44 cases.
Beyzadeoglu T, Pehlivanoglu T, Yildirim K, Buldu H, Tandogan R, Tuzun U.
The Orthopaedic Journal of Sports Medicine
First published Feb 20, 2020: https://doi.org/10.1177/2325967120902013
This research was undertaken by Professor Tahsin Beyzadeoglu, who is one of the leading Knee Surgeons in Turkey. This observational case-controlled cohort study looked at 44 patients having ACL reconstructions with hamstring autografts, with half having the graft sprayed with Vivostat PRF at the end of the procedure and half not. The patients were assessed post-operatively with MRI at the 5-month post-op point. In this study, the application of PRF to the ACL graft was shown to lead to superior graft integration and maturation in the proximal third of the graft, with a more normal signal intensity in the proximal graft and with less synovial fluid seen around the graft-tunnel interface. In addition, there were significantly fewer cases of post-operative haemarthrosis seen in the Vivostat PRF group.
Knee replacement surgery
Knee replacement surgery involves cutting the end 1/2cm or so of bone off the surfaces of a joint and replacing them with metal surfaces that are cemented onto the bone, with a very hard plastic ‘washer’ in between. To get into the knee one has to cut through the tissue layers at the front of the joint. These tissue layers plus the actual cut bone surfaces themselves all tend to bleed during and after the operation, which makes the knee joint swollen and painful.
Vivostat PRF is now used in knee replacement surgery as a fibrin sealant. The PRF is sprayed over any residual raw bone surfaces at the end of the procedure and also over the edges of the cut soft tissues, sealing the tissues and reducing bleeding. The Vivostat PRF thereby reduces post-op swelling and post-op pain, which makes the early post-operative period more comfortable and the post-op rehab easier.
Centre of Excellence
Mr McDermott was the first surgeon in the UK to use Vivostat PRF in a knee, and at the time of writing, Mr McDermott has performed over 300 knee cases where Vivostat PRF has been used.
Mr McDermott is now a designated ‘Vivostat Centre of Excellence’ for the use of biological glues in knee surgery, and he is a training centre for other surgeons to visit and to learn more about the use of Vivostat PRF.
CLICK HERE to read more