#treatment
ACL reconstruction
- The anterior cruciate ligament (ACL) is the main ligament at the front of the middle of the knee that stops the shin bone from wobbling too far forwards.
- The ACL also has a role in preventing rotational instability.
- ACL tears are relatively common in football, skiing or netball injuries, and tend to occur when the knee is twisted in a bent position, often in combination with impact/running.
- The immediate result of an ACL tear is severe pain and swelling in the joint.
- The longer-term results of having ACL deficiency in the knee are increased laxity (wobble), potential functional instability (giving way), an increased risk of subsequent meniscal cartilage tears and an increased risk of arthritis in the knee.
- If a patient is a high level or keen athlete/sportsman (particularly if their sport involves impact and pivoting) then they are likely to need an ACL reconstruction sooner rather than later.
- If a patient is lower demand, then it might be appropriate for them instead to undergo an extensive period of physiotherapy rehab, to try and strengthen up the muscles around the knee and speed up the reflexes, to try and compensate for the missing ligament. If they then do well then they may be able to avoid a surgical ligament reconstruction. If they do poorly, then the patient may then need to go ahead with an ACL reconstruction.
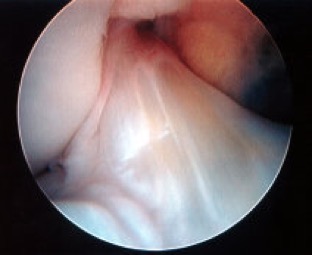
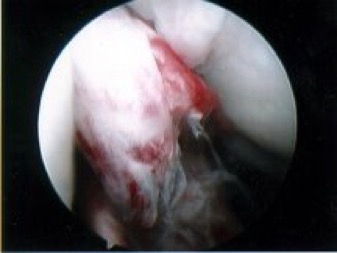
- When the ACL tears it is like a bungee rope snapping inside the knee, and the torn ends tend to ping apart. The torn ends also tend to be ragged, like the frayed ends of a rope. Unfortunately, direct repair of a torn ACL is rarely ever actually feasible (with the exception of one special case, which is a ‘tibial ACL attachment site avulsion fracture’). Therefore, instead the damaged ligament has to be replaced with a new ligament, i.e. a reconstruction.
- ACL reconstruction is a highly successful operation. A ‘graft’ is taken, which is normally a ligament taken from elsewhere (either from somewhere else in the patient’s own body, = an ‘autograft’, or from a donor, = an ‘allograft’).
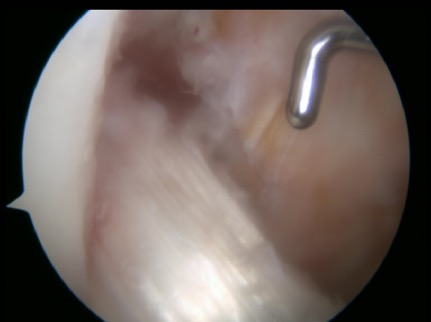
- Narrow tunnels are drilled through the tibia (shin bone) and the femur (thigh bone) into the middle of the knee. The ligament graft is passed up these tunnels, fixed at the top, tensioned and then fixed under tension at the bottom, to give a new tight ligament in the knee.
- With time, the new ligament grows a new blood supply in the knee, and the graft becomes a living structure within the patient’s knee.
- Rehab after an ACL reconstruction is slow. Cruthces are normally needed for just the first couple of days. Patients tend not to need a knee brace post-op unless other specific procedures have also been undertaken in the knee at the same time (eg meniscal repair). Regular physio treatments will be needed, and particular from 3 months onwards patients are encouraged to spend lots of time in the gym doing specific exercises. Patients should not return to sport until 9 months post-op.
- The success rate (from patient satisfaction scores) for ACL reconstruction is in the region of 90 to 95%.
Read more...
Rupture of the ACL is a very painful knee injury, which is normally fairly debilitating. With time, over several weeks, most knees begin to settle down from the initial injury. However, many patients are then left with a ‘wobbly’ knee that does not feel secure, and which is functionally unstable with intermittent episodes of giving way, particularly with impact and pivoting manoeuvres and sport.
Many people with an ACL rupture end up requiring surgery, to reconstruct the torn ligament. When the ACL tears it is like a tight bungee rope snapping in the knee. The torn ends tend to be shredded, like a frayed rope, and the stumps retract and scar up very quickly. In addition, the inside of the knee joint is filled with synovial joint fluid, which washes away any blood clot that the body might try to form between the torn ligament ends. Therefore, with the vast majority of ACL tears one cannot actually perform a primary/direct repair of the actual torn ligament, and instead the ligament needs to be replaced (reconstructed) with a new fresh ligament. [The one notable exception to this is the ACL tibial attachment avulsion fracture, where the ligament pulls a chunk of bone off the top of the tibia, from where it is attached. If this specific type of injury is caught quickly, then the bone chunk with the ligament still attached can be fixed back in place with a screw or wires, which normally allows the ligament to heal up well.]
How is an ACL reconstruction performed?
To replace a torn/missing ACL, one has to put a new ligament into the knee, and this is called a graft. The operation is performed under a general anaesthetic and tends to take about 1 hour (or longer if there are other things that need to be sorted out inside the knee at the same time). Most patients stay in hospital for just 1 night after the operation, and go home the following morning.
To place the graft properly in the knee, we drill a tunnel from the front of the tibia (shin bone) into the middle of the knee. We also drill a tunnel in the end of the femur. The graft is passed up the tibial tunnel, across the middle of the knee where the ACL used to sit, and then up the tunnel in the femur. We fix the graft in the femoral tunnel using a very small but extremely strong metal anchor. The graft is then tensioned and fixed under tension using a screw that is placed in the tibial tunnel.
The following animation shows how ACL surgery is performed:
Graft options
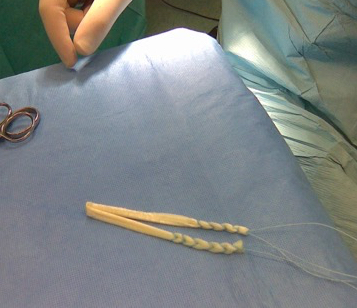
There are a number of different options available for what one can use as a graft to replace/reconstruct the ACL. These include:-
- 4-strand hamstring tendon from your own knee (autograft)
- bone-patellar tendon-bone composite graft from the front of your own knee (autograft)
- synthetic (artificial) graft
- allograft (a donor tendon graft)
CLICK HERE for further information about the graft options for ACL reconstruction.
ACL rehab
The rehab after an ACL reconstruction is just as important as the actual surgery.
If an isolated ACL reconstruction is performed, without other concomitant procedures such as meniscal repair, microfracture or articular cartilage grafting, then the early recovery is normally very quick. Most people are able to fully weight bear straight away, the first morning after their op, but with the help of crutches for comfort/safety for the first few days.
We normally advise patients to take things easy and just potter around for the first week or so, avoiding any long walks or any kind of proper exercise. The hospital in-patient phsyios will, however, see you on the ward prior to your discharge, to explain to you exactly what gentle exercises you can do and how to do them, and you will be given an advice booklet.
We usually see patients back in clinic at about 10 days post-op, to check that their knee is OK, to remove any stitches and to go through everything about the operation in detail with the patient (we provide full copies of the operation notes, the operation letter, the pictures of the operation from the inside of the knee, and the actual video of the operation – which you don’t have to watch if you don’t want to!)
After the post-op visit, patients are then ready to start regular, intensive physiotherapy rehab treatments (ideally 2 or 3 times a week), to get their knee going, to get the movement back in the joint, to get the strength back in the muscles and to re-train the reflexes.
Most patients are ready to start gentle jogging on a treadmill by 3 months post-op. Patients can then progress to pivoting/cutting type manoeuvres as soon as their neuromuscular strength and control is good enough, under the watchful guidance of their physio. Next comes sport-specific training. Finally, return to full sports can commence from 9 months post-op onwards.
So, the operation takes just 1+ hours, you are only in hospital for 1 night post-op, but the rehab actually takes a full 9 months! This is not, however, 9 months of doing nothing – far from it … it is 3+ months of hard regular work with the physios followed by 6 months of regular hard fitness and strengthening work in the gym. Quite often patients say that by the end of their rehab they actually feel fitter and stronger than they’ve ever felt before, because the injury and rehab has actually forced them to go to the gym on a regular basis.
The results of ACL reconstruction
About 90% of patients are entirely happy with the outcome of their surgery after an ACL reconstruction.
It should be noted that, as with any kind of surgical procedures, there are some potential risks with surgical ACL reconstruction. These include potential infection, nerve or blood vessel damage or blood clot formation such as a DVT (deep vein thrombosis) or PE (pulmonary embolus), which can potentially be very serious. However, thankfully, these complications are actually pretty rare.
One other interesting statistic is that about 10% of patients will end up rupturing their new ACL graft after a reconstruction, within the first 10 years. However, very interestingly, about 10% of patients with an ACL rupture will actually also rupture the ACL in their other knee too. This therefore suggests that perhaps some people are just simply prone to tearing their ACLs – and this may be partly genetic (the shape of the knee or the strength of the ligaments) and perhaps partly because the type of person who ruptures their ACL tends to be the more sporty, active kind of person who actually does higher risk activities. Still, it’s better to be fit and active and have fun and rupture your ACL (which can be reconstructed) than to be inactive, fat, unfit and die young of a heart attack!